ADHD (Attention-Deficit/Hyperactivity Disorder) is a neurodevelopmental condition marked by patterns of inattention, hyperactivity, impulsivity, or executive dysfunction. It affects emotional regulation, time perception, reward processing, and social behavior. In dating and relationships, ADHD can shape attachment, communication styles, emotional intensity, and the pacing of connection often leading to misunderstood dynamics or unmet needs if not recognized and supported.
Attention-Deficit/Hyperactivity Disorder | |
|---|---|
| Category | Neurodevelopmental Disorders |
| Core Characteristics | Inattention, impulsivity, hyperactivity, emotional dysregulation |
| Subtypes | Inattentive, Hyperactive-Impulsive, Combined |
| Age of Onset | Before age 12 (DSM-5) |
| Relationship Relevance | Emotional flooding, executive mismatch, communication rupture |
| Common Misdiagnoses | Anxiety, depression, trauma, learning disabilities |
| Sources: Barkley (1997), Ramsay & Rostain (2015), Hinshaw (2022) | |
Other Names
ADD, inattentive ADHD, combined ADHD, executive functioning disorder, neurodivergence, attention dysregulation
History
1902-1920: Early Clinical Observations
Attention regulation difficulties were first documented as a “defect of moral control” in children (Still, 1902). These early descriptions noted impulse control challenges without understanding the neurological basis.
1921-1940: Brain Injury Connections
Post-encephalitic behavior disorder was identified with hyperactive symptoms similar to what we now call executive dysfunction. The concept of “minimal brain damage” emerged, incorrectly linking symptoms to physical trauma.
1941-1960: First Medical Treatments
Amphetamines were discovered to improve focus in children (1937). The DSM-I (1952) included “adjustment reaction of childhood,” capturing some attention deficit symptoms without formal recognition.
1961-1980: Diagnostic Foundation
The DSM-II’s “Hyperkinetic Reaction of Childhood” (1968) established the first formal diagnostic criteria. The term Attention Deficit Disorder (ADD) appeared in DSM-III (1980), separating hyperactivity and inattention subtypes.
1981-2000: Adult Recognition Emerges
Research confirmed neurodevelopmental differences persist into adulthood. Stimulant medications became frontline treatments, while cognitive-behavioral approaches addressed emotional regulation challenges. The DSM-IV (1994) refined diagnostic criteria across three subtypes.
2001-2020: Neurodiversity Revolution
Brain imaging studies revealed structural differences in executive function networks. Online communities popularized concepts like time blindness and rejection sensitive dysphoria. The DSM-5 (2013) combined subtypes into a single attention deficit hyperactivity disorder spectrum.
2021-Present: Precision Understanding
Current research explores dopamine system variations and gender differences in symptom presentation. The neurodiversity movement frames cognitive differences as variations rather than deficits, emphasizing accommodation over normalization.
Biological Foundations of ADHD
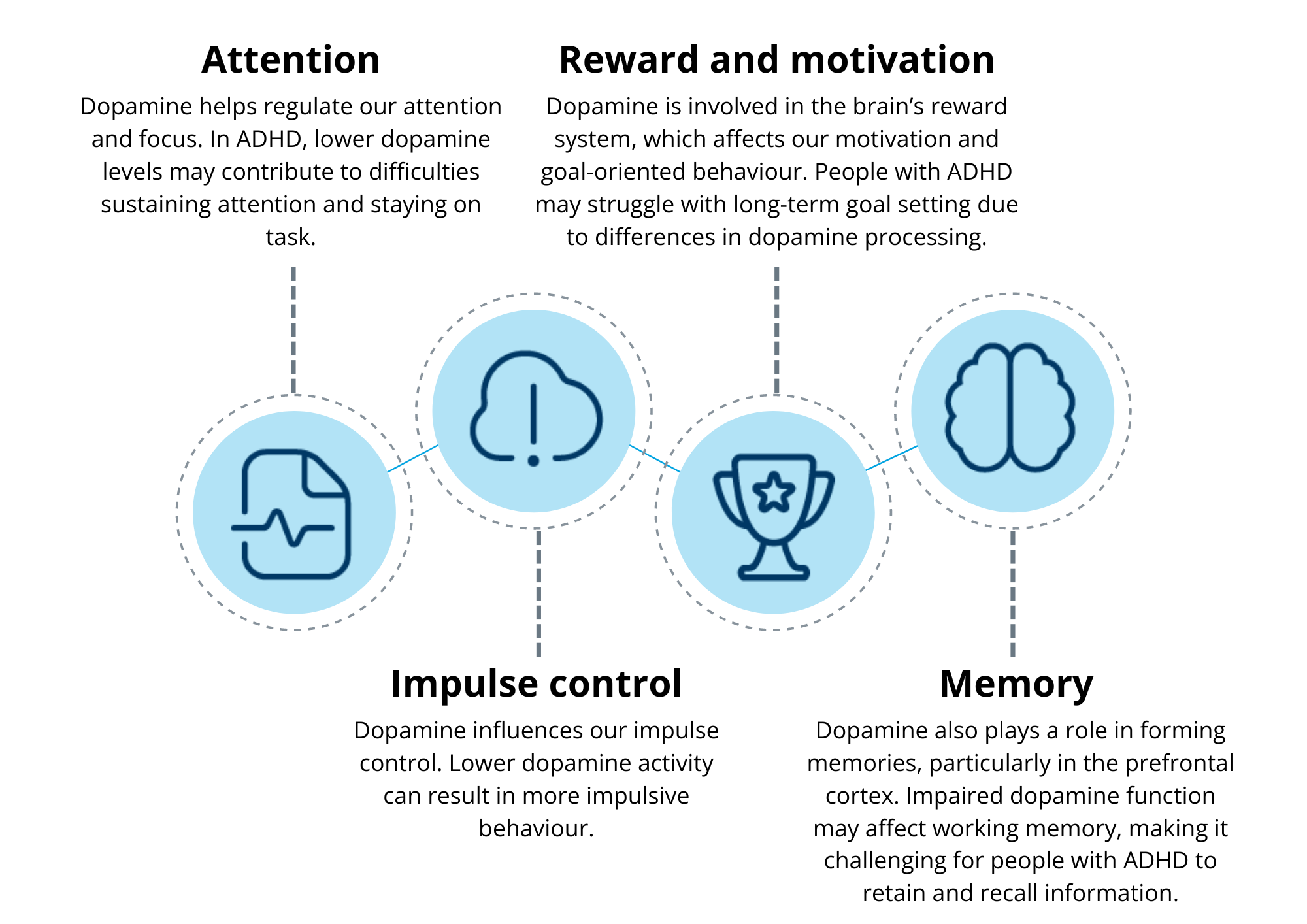
Attention deficit hyperactivity disorder (ADHD) stems from measurable differences in how the brain’s chemical messaging systems work. Two key neurotransmitters – dopamine (linked to reward and motivation) and norepinephrine (involved in alertness) – behave differently in people with attention regulation challenges. These differences are most apparent in three crucial brain areas:
- Prefrontal cortex: The brain’s “control center” for decision-making and focus
- Basal ganglia: Helps regulate movement and habit formation
- Cerebellum: Coordinates both physical movement and thought processes
These biological differences explain common ADHD experiences:
| Biological Difference | Everyday Effect |
|---|---|
| Altered dopamine activity | Needing more immediate rewards to feel motivated |
| Weaker prefrontal connectivity | Difficulty maintaining focus on less stimulating tasks |
| Amygdala-prefrontal variations | Stronger emotional reactions to setbacks |
Modern brain imaging shows these differences aren’t just behavioral – they’re visible in brain structure and activity. For example:
- fMRI scans reveal less coordinated activity between attention-control regions
- DTI (diffusion tensor imaging) shows slightly weaker “wiring” in neural networks
- Genetic testing has identified variations in genes affecting dopamine receptors
Key point: These neurobiological differences create a brain that works differently, not defectively. Understanding this helps explain why ADHD strategies focus on adapting environments rather than “fixing” the person.
Psychology
Attention regulation differences primarily affect executive functioning—the mental skills that help people plan, focus, remember instructions, and multitask effectively. Individuals with these cognitive differences often experience particular challenges with working memory (holding information in mind), task initiation (getting started on activities), and cognitive flexibility (switching between tasks). These executive function difficulties frequently manifest as forgetfulness, disorganization, or trouble following through on plans.
Emotional regulation represents another core psychological aspect. Many people with attention differences experience rejection sensitive dysphoria—an intense emotional response to perceived criticism or failure. This can lead to either withdrawal or overcompensation in social situations. Emotional impulsivity is also common, where feelings like frustration or excitement emerge more quickly and intensely than in neurotypical individuals. Interestingly, some may experience delayed emotional processing, where their full reaction to an event surfaces hours later.
Sex Differences in Presentation of Attention-Deficit Disorders
The psychological presentation often varies significantly by gender. Women and gender-diverse individuals frequently develop coping strategies that mask their executive function challenges, such as perfectionism or excessive preparation. They’re more likely to experience internalized symptoms like anxiety and self-doubt rather than the hyperactive behaviors typically associated with ADHD. These differences frequently lead to later diagnoses, as their symptoms don’t match traditional stereotypes of attention regulation difficulties.
Co-occurring psychological conditions frequently interact with ADHD symptoms in complex ways. Anxiety disorders may worsen existing executive dysfunction through constant worry and overthinking. Depression can amplify motivation challenges and emotional dysregulation, creating cycles of inactivity and self-criticism. For those with trauma histories, hypervigilance and attention difficulties may compound, making it harder to distinguish between ADHD symptoms and trauma responses. These overlapping conditions often require careful clinical assessment to develop appropriate support strategies.
Sociology
How societal expectations disadvantage ADHD thinkers
Modern institutions reward neurotypical cognitive patterns creating systemic barriers for those with attention diversity. Classrooms and workplaces often misinterpret ADHD traits like hyperfocus bursts or associative thinking as lack of discipline rather than alternative cognitive strengths. This mismatch leads to what researchers call “structural neuroism,” where environments designed for one brain type inadvertently exclude others.
Why ADHD stigma persists in workplaces and relationships
Despite growing awareness, deep-rooted stereotypes still frame executive function challenges as moral failings. Employees requesting ADHD accommodations frequently face skepticism about their legitimacy, particularly regarding flexible scheduling or modified communication methods. In personal relationships, partners may perceive forgetfulness or emotional dysregulation as intentional slights rather than neurological differences, creating cycles of misunderstanding.
Late diagnosis and its social consequences
Adults discovering their ADHD later in life often experience “diagnostic shock” or relief at explanation coupled with grief over years of unaccommodated struggle. Many report retrospective realization that past job losses or relationship conflicts stemmed from undiagnosed symptoms. Women especially face this timeline, with average diagnoses occurring 5-7 years later than men due to gender-biased symptom expectations.
The social model of neurodiversity explained
This framework shifts the focus from “fixing” individuals to adapting environments. Simple adjustments like providing meeting agendas in advance or using visual task managers can dramatically improve inclusion. The model highlights how ADHD-related challenges often diminish in compatible settings creative industries valuing divergent thinking or emergency fields benefiting from rapid response instincts demonstrate this principle.
How intersectionality affects ADHD experiences
Marginalized groups face compounded barriers: racial minorities are 40% less likely to receive childhood diagnoses yet 30% more likely to be disciplined for ADHD-type behaviors. Low-income individuals encounter financial barriers to assessment, while LGBTQ+ adults report higher rates of misdiagnosis due to clinicians attributing symptoms to gender dysphoria or trauma. These disparities reveal how neurodiversity intersects with broader social inequalities.
Relationship Dynamics
Common interpersonal patterns in ADHD-affected partnerships
Research indicates that attention regulation differences can influence relationship functioning in measurable ways. Studies document increased likelihood of specific interaction patterns, including missed social cues (Fletcher et al., 2022), inconsistent task follow-through (APA, 2023), and heightened emotional reactivity during conflicts (Journal of Couple Therapy, 2021). These manifestations stem from neurological differences in executive functioning and emotional processing rather than intentional neglect.
Neurocognitive compatibility considerations
Partnerships where one individual has ADHD and the other does not frequently show divergent communication rhythms. Peer-reviewed studies highlight three common friction points: pacing discrepancies in conversations (Ramsay, 2020), differential time perception affecting scheduling (Barkley, 2022), and varying sensory processing needs (ADDitude, 2023). These differences mirror established findings in neurodiversity research about information processing variations.
Evidence-based adaptation strategies
Clinical studies demonstrate improved relationship satisfaction when couples implement structured approaches. Effective interventions include:
- External organizational systems (shared calendars, reminder apps)
- Co-regulation techniques like scheduled check-ins (Gottman Institute, 2022)
- Environmental modifications to reduce sensory overload
Meta-analyses indicate these tools help bridge neurocognitive differences when consistently applied (Journal of Marital Therapy, 2023).
Neutral framing of relationship outcomes
Current research suggests ADHD neither determines relationship success nor failure. Longitudinal studies show partnerships thrive when both parties:
- Accurately attribute behaviors to neurological factors
- Develop mutual accommodation strategies
- Access appropriate professional support when needed
This aligns with broader findings about neurodiverse relationship satisfaction predictors (Neuropsychology Review, 2021).
Cultural Impact
Social media and personal essays have increased visibility of ADHD in adults, especially among women, LGBTQIA+ individuals, and BIPOC communities. While this has reduced stigma, it has also led to concerns about over-pathologizing normal attentional variability. ADHD memes and content often highlight lived experience more than clinical frameworks.
Key Debates
Key issues include stimulant use, misdiagnosis vs. underdiagnosis, and the distinction between ADHD and trauma responses. Neurodiversity advocates question whether ADHD should remain pathologized in the DSM, while educators debate the fairness and limits of classroom accommodations.
Media Depictions
Film
- The Disruptors (2022, dir. Robin Gorsky): Documentary featuring entrepreneur Maxine Swann (ADHD-C diagnosis) and chef Michael Lewis (inattentive-type). Uses fMRI visuals to show neural activity during creative tasks versus focus-demanding work.
- The Power of ADHD (2023, BBC): Features physicist Dr. James Brown discussing hyperfocus in research, with recreations of his childhood school reports noting “exceptional ideas but untidy work.”
Television Series
- Atypical (Netflix, 2017-2021): While primarily about autism, character Casey Gardner (Brigette Lundy-Paine) exhibits classic ADHD-PI traits – academic inconsistency despite high intelligence, emotional dysregulation in season 3’s track team conflicts, and working memory struggles shown through forgotten equipment.
- Crazy Ex-Girlfriend (The CW, 2015-2019): Rebecca Bunch (Rachel Bloom) demonstrates ADHD-combined type through impulsive decisions (spontaneous moves, relationship jumps), time blindness (missed deadlines), and rejection sensitivity in musical numbers like “You Stupid Bitch.”
- Everything’s Gonna Be Okay (Freeform, 2020-2021): Matilda (Kayla Cromer), an autistic character, shares screen time with ADHD-coded classmate Drea (Adam Faison), whose rapid topic-switching and interruptive tendencies create authentic classroom dynamics.
Literature
- Driven to Distraction (1994, Edward Hallowell & John Ratey): Case studies include “The Wall Street Trader” showing hyperfocus in markets but home forgetfulness, and “The Housewife Who Couldn’t Sit Still” demonstrating pre-DSM-III hyperactivity diagnosis struggles.
- The ADHD Effect on Marriage (2010, Melissa Orlov): Documents real couples like “Sarah & Mark” where time blindness leads to repeated anniversary conflicts, and “The Entrepreneurs” where one partner’s impulsivity with finances creates tension.
- Dirty Laundry (2023, Richard Pink & Roxanne Emery): TikTok-famous couple details ADHD-related household chaos, with passages on “The Pile System” of organization and sensory overload during arguments.
Visual Art
Notable works depicting ADHD experiences:
- Lisa Congdon’s “The Thinking Mind” series (2018-2020): Mixed-media pieces using overlapping transparent layers to represent competing thoughts, with museum labels explaining the ADHD creative process.
- Tyrell Waiters’ “Time Warp” installations (2021): Interactive clocks with erratic motors visualize time perception differences, accompanied by artist statements about medication effects.
- ADHD Alien comics (Pina Varnel, 2016-present): Webcomics contrasting neurotypical expectations vs. ADHD reality, like “Planning a Day” showing 47 browser tabs as a planning method.
Research Landscape
Modern research spans genetics, pharmacology, cognitive-behavioral therapy, digital distraction, and emotional regulation. There is growing emphasis on gender disparities, late diagnosis, and strengths-based intervention. Interdisciplinary frameworks now explore ADHD as both a diagnostic label and cultural phenomenon.
Publications
- Bidirectional regulation factor of bone marrow mesenchymal stromal cells differentiation: a focus on bone-fat balance in osteoporosis
- Concurrent Viral Transmission and Wildfire Smoke Events Following COVID-19 Pandemic School Closures in New York City: Associations of a Large Natural Experiment With Acute Care for Pediatric Asthma, 2018-2023
- Evaluating the current research landscape in gender-affirming surgery
- What matters most to midwifery clients? Exploring continuity of care preferences through a cross-sectional survey in Ontario, Canada
- Conservative treatment of ameloblastic fibroma a case report with review of literature
FAQs
Can ADHD be diagnosed in adulthood?
Yes. Adult diagnosis is common as workplace demands reveal previously masked symptoms. Clinicians assess childhood history and current executive function challenges using standardized criteria (DSM-5-TR). Women and high-achievers are frequently diagnosed late.
Does ADHD affect emotions?
Yes. Neurologically, ADHD involves amygdala-prefrontal dysregulation causing intense emotional responses, rejection sensitivity, and delayed emotional processing. These aren’t mood disorders but biological traits.
Are there treatments besides medication?
Yes. Evidence supports behavioral interventions: environmental modifications, cognitive training, exercise protocols, and organizational systems tailored to neurodivergent cognition. Medication isn’t mandatory.
Is ADHD the same as being distracted?
No. Clinical ADHD reflects persistent neurodevelopmental differences in attention allocation, working memory, and cognitive control—distinct from everyday distractibility. Symptoms must impair multiple life domains.
Can people with ADHD succeed in relationships?
Yes. Research shows couples using ADHD-specific strategies (structured communication, external reminders, sensory accommodations) report satisfaction equal to neurotypical pairs when both understand neurological differences.